Causes
Skin lesions from pityriasis rosea occur with equal frequency in men and women. Therefore, these skin changes are not hormonal in nature. The highest incidence rate is observed in the autumn-winter period, when a person’s skin is hidden under warm clothing.
The following diseases and pathological conditions contribute to the appearance of plaques:
- weakened immunity due to chronic diseases;
- metabolic diseases;
- helminthic infestation;
- state of chronic stress;
- presence of allergic diseases.
With pityriasis rosea, the surface layer of the skin, the epidermis, is affected, and the middle layer, the dermis itself, becomes thinner. As a result, the skin in the affected area becomes thinner, the blood vessels become visible, giving a pink tint. Then, ridges form along the edges of the plaque, limiting the focus of pathological changes. The epithelium is sloughed off and replaced with new cells. At the site of the lichen, a pale spot remains for some time, which rather acquires a normal flesh color.
Which doctor should I contact?
For classic herpes zoster with skin rashes, a consultation with an ID-Clinic dermatologist is required. The doctor will conduct an initial diagnosis and, if necessary, give a referral to a neurologist or infectious disease specialist. To make a diagnosis, the patient will need to undergo an extensive examination.
Taking into account the results obtained, the doctor selects an individual treatment regimen using antiherpetic drugs, painkillers and other medications. With timely initiation of therapy, the prognosis is favorable.
Symptoms
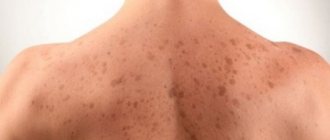
The appearance of pink spots on the skin occurs in strict sequence. Only with Zhiber's lichen does a maternal plaque first appear - an ovoid-shaped spot the size of a quail egg, pink in color, with clear edges. Within two to three days, a rim of darker color forms along the edges of the maternal plaque, and the skin on the surface of the spot becomes flaccid, similar to tissue paper. Then the epithelial cells begin to slough off and be rejected.
After a few days, in places far from the “maternal plaque”, new spots appear, which also have clear outlines, but are smaller in size. The number of fresh plaques is sometimes impossible to count. But the foci of pityriasis rosea never merge, maintaining clear boundaries. The skin in the areas of daughter rashes undergoes the same changes as in the maternal plaque.
The disease is not accompanied by any sensations. No itching, pain, swelling. General changes in the body are limited to an emotional reaction to the appearance of a large number of spots. In the absence of medical care, plaques resolve on their own without dangerous consequences or complications.
The disease is prone to relapse in cases where the background condition of the body does not change or a chronic disease (for example, bronchial asthma) cannot be completely cured.
Atypical forms of the disease
In some cases, the course of herpes zoster differs from the classical pattern, which makes timely diagnosis difficult. There are several forms of Herpes zoster:
1. Abortive. It has minimal clinical manifestations: malaise, weakness, redness and swelling of the skin without rashes. The duration of the illness does not exceed several days.
2. Bullous. Skin symptoms include flaccid blisters the size of a pea or larger, which are filled with clear fluid. This type of herpes zoster is accompanied by severe intoxication.
3. Hemorrhagic. Develops in patients with a suppressed immune system. In this case, the lesion affects the deep layers of the skin: the blisters are filled with bloody contents, and dark brown crusts appear.
4. Gangrenous. Another variant of Herpes zoster, typical for elderly and weakened patients. Skin inflammations do not heal for a long time, turning into ulcers that leave behind rough scars.
5. Generalized. It is characterized by the spread of a herpetic rash over a large area of skin beyond the zone of innervation of one nerve. This form is observed in immunocompromised patients.
Treatment
Treatment of pityriasis rosea is carried out according to the general rules for the treatment of skin diseases. Since changes in the skin do not have a pronounced inflammatory reaction, the use of local drugs is sufficient. First, drugs with keratolytic activity are used, and then drugs with keratoplastic activity. The first ones loosen the epidermal cells, accelerating their rejection. The latter enhance the processes of skin cell regeneration.
Pharmacological agents are replaced at a time when the affected cells are exfoliated and a new layer of skin surface begins to form. A dermatologist monitors the treatment and makes the right decision on time.
Refusal of any medical measures delays the course of the disease up to 3-6 months, while the course of treatment usually lasts no more than 10-14 days.
Shingles
Shingles (herpes zoster) is a common human disease that is characterized by general infectious symptoms, skin manifestations and neurological disorders of the central and peripheral nervous system.
The disease is caused by the Varicella zoster virus, which is also the causative agent of chickenpox. The virus contains DNA, being neurodermotropic, it affects the skin, cells of the central and peripheral nervous system. The virus is unstable in the external environment: it quickly dies when heated, under the influence of ultraviolet rays and disinfectants. It lasts for a long time at low temperatures.
Initially or after chickenpox, the virus penetrates through the skin and mucous membranes, then through the lymphogenous and hematogenous route into the intervertebral nodes and dorsal roots of the spinal cord, where it can persist for a long time in a latent state. With a decrease in immunological reactivity under the influence of various factors, such as exacerbation of chronic diseases, taking immunosuppressants, intoxication, latent infection, it can become more active. Herpes zoster is most severe in patients with cancer, HIV-infected people, as well as in people who have received corticosteroids or radiotherapy. Activation of the virus is accompanied by the development of ganglioneuritis with damage to the intervertebral ganglia or ganglia of the cranial nerves, as well as the dorsal roots (E. S. Belozerov, Yu. I. Bulankov, 2005). In severe cases, the anterior and posterior horns, white matter of the spinal cord, and brain may be involved in the process. The virus can also infect the autonomic ganglia, causing dysfunction of internal organs.
Pathomorphological changes in the brain with lesions of the central nervous system can be varied. In mild cases, changes occur only in the spinal cord and root ganglia; swelling is recorded in the brain. In severe cases, pronounced infiltration of the subarachnoid space, cerebral edema, hemorrhage in the white matter, basal ganglia and brain stem are noted.
The incubation period for herpes zoster can be several years from the moment of infection. In the clinical course, the main ones are: the prodromal period, the period of clinical manifestations and the period of residual effects. It all starts with an increase in temperature, a tingling sensation, burning, itching at the site of the rash, and a headache. Along the nerve trunks of the trunk, limbs or head, limited pink spots up to five centimeters in diameter appear. On the second day, bubbles 2–3 mm in diameter appear, filled with transparent contents. The number of lesions can vary from one to several, closely adjacent to each other, forming a continuous line. Over time, the contents of the bubbles become cloudy. At about 8–10 days, the blisters dry out and crusts form, which disappear after 3–4 weeks. In many patients, neurological manifestations can last for several months (up to a year).
Typical clinical manifestations of herpes zoster are characterized by a certain sequence of skin rashes. The rashes are segmental, unilateral and do not spread to the other side of the body, unlike chickenpox.
Lesions of the nervous system with herpes zoster occupy first place among the complications of this disease. In the structure of neurological disorders, the leading place is occupied by lesions of the peripheral nervous system [10]. The most common disorders are neuralgia, neuropathy of the cranial and peripheral nerves, serous meningitis, etc. The most common manifestation is pain in the area of skin rashes. The pain is paroxysmal in nature, intensifying at night. In the future, the pain may intensify and bother you for several months and even years. Herpes zoster can also occur only with the symptoms of radicular pain, which is not preceded by a period of rash.
Most often, the rashes are located on the skin of the torso and limbs. The localization of pain and the appearance of a specific rash correspond to the affected nerves, most often intercostal nerves and are encircling in nature. The intensity of the pain increases with the slightest touch to the skin, with movement, or temperature changes. After the blisters disappear, the erosions epithelialize, and temporary red or red-brown pigmentation may remain on the skin. Some patients may have no pain. And sometimes herpes zoster can manifest itself only as neurological symptoms without the absence of skin manifestations.
Very often the localization of the disease is the skin of the face and head, especially the branches of the trigeminal nerve. Manifestations of the disease begin acutely, with general symptoms of intoxication and fever. Some patients may experience facial paralysis and trigeminal neuralgia lasting up to several weeks.
There may be manifestations of motor functions that occur not only when herpes zoster is localized in areas of the skin innervated by cranial nerves, but also when the cervical, thoracic and lumbar spinal cord, roots and ganglia are involved. Almost 5% of patients with rashes of various locations experience paresis of the upper and, more often, lower extremities, which indicate the phenomenon of focal myelitis.
To understand the pathogenesis of herpes zoster, data from pathological studies are important, indicating a connection between areas of the rash and damage to the corresponding ganglia. Head and Campbell (1900), based on pathohistological studies, came to the conclusion that both the neurological phenomena of herpes zoster and the areas of skin rashes that characterize them arise as a result of the development of a pathological process in the spinal nodes and their homologues (Gasserian node, etc.). But Volville (1924), having studied the nervous system of patients who died from a generalized form of herpes zoster, came to the conclusion that damage to the intervertebral ganglia in herpes zoster is not necessary. The inflammatory process often involves the spinal cord, and not only the posterior horns are affected, but also the anterior ones. Volville and Shubak (1924) described cases in which herpetic rashes were the first manifestations of a polyneurotic process occurring like Landry's paralysis. Volville believes that the inflammatory process first affected sensory neurons, and then spread to the spinal segments and peripheral nerves. In the case described by Shubak, a pathological examination revealed nests of inflammatory infiltration in the sciatic nerves, cervical sympathetic ganglia and the corresponding spinal ganglia, and the dorsal horns of the spinal cord.
Thus, the process involves not only the spinal and cerebral ganglia, which are most often affected, but also the substance of the spinal (anterior and especially posterior horns, white matter) and brain (oblongata, pons, hypothalamic region) brain, as well as the meninges.
Pathological and virological studies indicate that the herpes zoster virus widely disseminates throughout the body. During illness, it can be isolated from the contents of vesicles, saliva, tear fluid, etc. This gives reason to believe that herpetic eruptions can be caused not only by the settling of the virus in the sensory ganglia and damage to the parasympathetic effector cells located in them, but also by direct penetration it into the skin. Penetrating into the nervous system, it is localized not only within the peripheral sensory neuron (spinal ganglia, etc.), but also spreads to other parts of the central nervous system. When it is introduced into motor cells and roots, a picture of amyotrophic radiculoplexitis arises; in the gray matter of the spinal cord - myelitic syndrome; into the cerebrospinal fluid system - meningoradiculoneuritis or serous meningitis, etc.
The clinical picture of herpes zoster consists of skin manifestations and neurological disorders. Along with this, most patients experience general infectious symptoms: fever, enlargement of hormonal lymph nodes, changes (in the form of lymphocytosis and monocytosis) and cerebrospinal fluid. Typically, erythematous spots of round or irregular shape, raised, swollen, are found on the skin; when running a finger over them, a certain shagreen-like appearance of the skin is felt (tiny papules). Then, in these areas, groups of bubbles appear successively, often of varying sizes. The bubbles can merge with each other, but most often they are located in isolation, although close to one another - the vesicular form of herpes zoster. Sometimes they look like a small bubble surrounded on the periphery by a red rim. Since the rash occurs simultaneously, the elements of the rash are at the same stage of their development. However, the rash may appear in separate clusters over 1 to 2 weeks. In the latter case, when examining the patient, rashes can be detected at various stages of evolution. In typical cases, the bubbles at first have transparent contents, which soon turn cloudy, and then dry out in the form of a crust. A deviation from the described type is a milder abortive form of herpes zoster. With this form, papules also develop in the foci of hyperemia, which, however, do not transform into vesicles, which is how this form differs from the vesicular one. Another type is the hemorrhagic form of herpes zoster. The blisters have bloody contents, the process spreads deeply into the dermis, the crusts become dark brown. In severe cases, the bottom of the vesicles becomes necrotic - a gangrenous form of herpes zoster, after which scarring changes remain. The intensity of the rashes in this disease is very variable: from confluent forms, leaving almost no healthy skin on the affected side, to individual blisters, although in the latter case the pain can be sharply expressed. Such cases have given rise to the assumption that herpes zoster may exist without a skin rash.
Skin manifestations correspond to the level of damage to certain vegetative formations. By localization, lesions of the following ganglia are distinguished: gasserian, geniculate, cervical, thoracic, lumbosacral. One of the leading symptoms of the disease are neurological disorders, usually in the form of pain. Most often it occurs 1–2 days before the rash appears. The pain, as a rule, is intense, burning in nature, and the area of its distribution corresponds to the roots of the affected ganglion. It should be noted that the pain syndrome intensifies at night and under the influence of a variety of stimuli (cold, tactile, kinesthetic, barometric) and is often accompanied by vegetative-vascular dystonia of the hypertensive type. In addition, patients experience objective sensitivity disorders: hyperesthesia - the patient can hardly tolerate the touch of linen, hypoesthesia and anesthesia, and hyperalgesia may exist simultaneously with tactile anesthesia. Objective sensitivity disorders vary in form and intensity, they are usually limited to temporary sensitivity disorders in the area of rash or scars. Anesthesia affects all types of sensitivity, but in some cases a dissociated type of disorder is observed; sometimes within the same type of sensitivity, such as hot and cold. Occasionally, hyperesthesia takes on the character of irritation in the form of causalgia. Not in all cases, the intensity of the pain syndrome corresponds to the severity of skin manifestations. In some patients, despite the severe gangrenous form of the disease, the pain is minor and short-lived. In contrast, a number of patients experience prolonged intense pain with minimal skin manifestations.
Some patients in the acute phase have diffuse cephalgia, which intensifies with changes in head position, which may be associated with a meningeal reaction to herpes zoster infection. According to a number of authors [11, 12], herpetic ganglionitis of the Gasserian ganglion is more common than ganglionitis of the intervertebral ganglion. Most patients with this localization of the process experience increased temperature and swelling of the face on the affected side, as well as pain at the exit points of the trigeminal nerve.
The cornea is often affected in the form of keratitis of various types. In addition, other parts of the eyeball are affected - episcleritis, iridocyclitis, iris zoster. The retina is very rarely involved (hemorrhages, embolisms), more often the changes affect the optic nerve - optic neuritis resulting in atrophy, possibly due to the transition of the meningeal process to the optic nerve. With ophthalmoherpes (iritis), glaucoma may develop; Usually, with zoster, hypotension of the eyeball is observed, which is apparently caused by damage to the ciliary nerves. Complications of zoster from the motor nerves are quite common and are located in the following order: III, IV, VI nerves. Of the branches of the oculomotor nerve, both external and internal branches are affected. Ptosis is often observed. Skin rashes with ophthalmic zoster are often more severe than on other parts of the body, possibly depending on the structure of the skin in the eye area. Quite often, necrosis of the vesicles and severe neuralgia, accompanied by lacrimation, are observed. Bubbles appear not only on the skin, but also on the mucous membranes of the eye. As a result of the process in the cornea with ophthalmic zoster, optic nerve atrophy and complete blindness can develop. In addition, some patients experience loss of eyebrows and eyelashes on the affected side. The maxillary branches of the trigeminal nerve are affected both in the skin and in the mucous membranes (half of the hard and soft palate, velum, upper gum, inner surface of the buccal mucosa, while the nasal mucosa may remain unaffected). The branches supplying the mucous membranes may be more affected than the cutaneous branches, and vice versa. Lesions of the nerves of the upper and lower jaws do not always remain strictly localized, since pain sometimes radiates to the area of the ophthalmic and other branches.
Herpes zoster usually affects the autonomic nervous system. However, clinical observations have shown that the animal nervous system may also be involved in the pathological process. Evidence of this is that some patients, simultaneously with damage to the Gasserian ganglion, had peripheral paresis of the facial nerve on the side of the herpetic rash. With ophthalmic zoster, both the external and internal muscles of the eye are paralyzed. IV paralysis is rare. Oculomotor paralysis is more often partial than complete; More often than other muscles, m. is affected. levator palpebrae. There are cases of ophthalmic zoster with isolated changes in the shape and size of the pupil; unilateral Argil-Robertson (Guillén) sign. These paralysis sometimes partially or completely resolve spontaneously without special treatment.
Simultaneous damage to the facial, auditory and trigeminal nerves was first described by Frankl-Hochwart in 1895. Hunt (1907) described in detail the four clinical forms of this disease, which later became known as Hunt's syndrome, or herpes zoster oticus. The defeat of the geniculate ganglion in this form of herpes zoster was first pointed out by Nordahl (1969). Usually, herpetic rashes appear on or around the ear, and sometimes in the ear canal and even on the eardrum. There is sharp pain in the circumference of the auricle. Dysfunction of the facial, cochlear, and vestibular nerves occurs in the first days of the rash or precedes it. Pain in such cases is localized in the depths of the ear canal and the auricle with irradiation to the mastoid region, auricular and temporoparietal areas.
Objective sensitivity disorders are found behind the ear, in the fold between the auricle and the mastoid process. This skin area is supplied by the auricular branch of the X pair, which innervates the posterior walls of the auditory canal. Finally, in cases of very common ear zoster, the latter affects not only the external auditory canal, the auricle, the mastoid process, but also the eardrum, which is sometimes extremely seriously affected. In such cases, the area innervated by pairs V, VII and X is affected, and damage to these nerves is accompanied by damage to the ganglia, corresponding cranial nerves, or anastomoses connecting the terminal branches of all of the above nerves.
Often, simultaneously with paralysis of the VII pair, there is paralysis of the soft palate, anesthesia and paresthesia in the tongue, and often a taste disorder in the anterior two-thirds of the tongue due to the lesion. The defeat of the VIII pair usually begins with tinnitus, which sometimes lasts a long time after the disappearance of other phenomena. Hyperacusis with damage to the VIII pair is caused by paresis n. stapeblii, although this symptom can also occur with isolated and previous damage to the auditory nerve and in such cases represents a symptom of irritation. Hypoacusis can occur regardless of damage to the auditory nerve due to local lesions of the middle ear, eruption of bubbles on the eardrum, blockage of the external auditory canal, due to swelling of the mucous membrane due to eruption of zoster.
Vestibulatory phenomena, in contrast to cochlear phenomena, usually develop extremely slowly and are expressed differently: from mild subjective symptoms of dizziness to significant static disorders.
Neuralgia with auricular zoster, as opposed to ophthalmic zoster, is rare. Long-term results are not always favorable, as persistent paresis of the facial nerve and deafness may occur.
Volville emphasizes that the combination of paralysis of the VII and VIII pairs, although it occurs especially often with zoster, nevertheless the same combination occurs when the Gasserian node, II, III, cervical ganglia are affected, and, finally, all of the above areas can be affected simultaneously.
Zoster rashes are also described in the area of innervation of the IX pair; the posterior part of the soft palate, the arch, the posterolateral parts of the tongue, part of the posterior wall of the pharynx; In addition to IX, this same area is also innervated by branches of the X pair: the root of the tongue, larynx, epiglottis, basal and posterior parts of the pharyngeal wall. Although zoster predominantly and even selectively affects the sensory systems, movement disorders are sometimes observed with it, especially when the rash is localized in the head, neck, and limbs. Paralysis with zoster is radicular in nature, and damage to the posterior roots in these cases is accompanied by phenomena from the corresponding anterior roots.
Damage to the cervical sympathetic nodes is often accompanied by rashes on the skin of the neck and scalp. Pain in this case is observed not only in places of rashes, but also in the area of paravertebral points. Sometimes attacks that mimic facial sympathalgia may occur.
With ganglionitis of the lower cervical and upper thoracic localization, along with the usual symptoms of this disease, Steinbrocker syndrome can be observed. The dominant picture of this syndrome is pain of a sympathetic nature in the form of burning or pressure, occurring initially in the hand, and then in the entire arm. Soon swelling of the hand appears and quickly increases, spreading to the entire arm. Trophic disorders are added in the form of cyanosis and thinning of the skin, hyperhidrosis, and brittle nails. Movement of the fingers is limited and painful. Often pain and other autonomic disorders persist even after the rash disappears. Thoracic ganglionitis often simulates the clinical picture of myocardial infarction, which leads to diagnostic errors.
With herpetic lesions of the ganglia of the lumbosacral region, the rashes are most often localized on the skin of the lower back, buttocks and lower extremities; Along with pain in the areas of rashes, pain syndromes simulating pancreatitis, cholecystitis, renal colic, and appendicitis may occur. Herpetic lesions of the lumbosacral ganglia are sometimes accompanied by involvement of the animal nervous system in the process, giving a picture of ganglioradiculitis (radicular syndrome of Pori, Matskevich, Wasserman).
Sometimes, along with rashes along the nerve trunk, vesicular rashes appear throughout the skin - a generalized form of herpes zoster. Usually the disease does not recur. However, it is known from the literature that recurrent forms of the disease occur against the background of somatic complications: HIV infection, cancer, diabetes mellitus, lymphogranulomatosis, etc.
Treatment . When treating herpes zoster of varying localization and severity, early administration of antiviral drugs is necessary. It is known that the virus contains proteins that form its shell and carry enzymatic functions, as well as nucleic acid, the carrier of its genetic properties. Penetrating into cells, viruses are freed from their protective protein shell. It has been shown that at this moment it is possible to inhibit their reproduction using nucleases. These enzymes hydrolyze the nucleic acids of viruses without damaging the nucleic acids of the cell itself. It was found that pancreatic deoxyribonuclease sharply inhibits the synthesis of DNA-containing viruses, such as herpes virus, vaccinia, and adenoviruses. Considering the above, it is recommended that patients with herpes zoster be prescribed deoxyribonuclease intramuscularly 1-2 times a day, 30-50 mg for 7 days. In addition, in patients with rashes on the oral mucosa, conjunctiva and cornea, the drug is used topically in the form of an aqueous solution. The administration of deoxyribonuclease promotes rapid regression of skin rashes and a reduction in pain.
The drug Isoprinosine has a good effect in the treatment of herpes zoster. This is an immunostimulating agent with an antiviral effect. Isoprinosine blocks the reproduction of viral particles by damaging its genetic apparatus, stimulates the activity of macrophages, the proliferation of lymphocytes and the formation of cytokines. The second component increases the availability of Isoprinosine for lymphocytes. Reduces the clinical manifestations of viral diseases, accelerates convalescence, and increases the body's resistance.
Indications: viral infections in patients with normal and weakened immune systems (diseases caused by herpes simplex viruses types 1 and 2, Varicella zoster, including chickenpox, measles, mumps, cytomegalovirus (CMV), Epstein-Barr virus); viral bronchitis; acute and chronic viral hepatitis B and C; diseases caused by the human papillomavirus; subacute sclerosing panencephalitis. Chronic infectious diseases of the urinary and respiratory systems; prevention of infections in stressful situations; the period of convalescence in postoperative patients and persons who have suffered serious illnesses; immunodeficiency states. Isoprinosine is taken orally, for adults - 50 mg/kg/day in 3-4 doses; for children - 50–100 mg/kg/day in 3–4 doses. Duration of treatment is 5–10 days, in severe cases up to 15 days. For diseases caused by herpes simplex viruses types 1 and 2, treatment is continued until the symptoms of the disease disappear and for another two days. For subacute sclerosing panencephalitis for adults and children - 50–100 mg/kg/day in 6 divided doses. For acute viral encephalitis for adults and children - 100 mg/kg/day in 4–6 divided doses for 7–10 days. This is followed by a break for 8 days, then a repeat course for 7–10 days. If necessary, the dose and duration of the continuous course can be increased, subject to a mandatory break in taking the drug for 8 days. Long-term treatment is carried out under medical supervision. For genital warts in complex therapy with a CO2 laser - 50 mg/kg/day in 3 divided doses for 5 days, then with a 3-fold repetition of the specified course at intervals of one month.
In recent years, antiviral chemotherapy drugs from the group of synthetic acyclic nucleosides have been used to treat herpes zoster. The most well studied drug at present is acyclovir. The mechanism of action of acyclovir is based on the interaction of synthetic nucleosides with the replication enzymes of herpes viruses. Thymidine kinase of the herpes virus binds to acyclovir thousands of times faster than cellular ones, so the drug accumulates almost only in infected cells. This explains the complete absence of cytotoxic, teratogenic and mutagenic properties in acyclovir. The synthetic nucleoside is arranged in a chain of DNA being built for the “daughter” viral particles, and this process ends in this way: the reproduction of the virus stops. The daily dose of acyclovir for herpes zoster is 4 g, which should be divided into 5 single doses of 800 mg. The course of treatment is 7–10 days. The best therapeutic effect is achieved with early administration of the drug; The duration of rashes is reduced, crusts form quickly, intoxication and pain are reduced. Second generation acyclovir - valacyclovir, retaining all the positive aspects of acyclovir, due to increased bioavailability, allows you to reduce the dose to 3 g per day, and the number of doses - up to three times. The course of treatment is 7–10 days. Famciclovir has been used since 1994. The mechanism of action is the same as that of acyclovir. The high affinity of the virus thymidine kinase for famciclovir (100 times higher than the affinity for acyclovir) makes the drug more effective in the treatment of herpes zoster. The drug is prescribed 250 mg 3 times a day for 7 days.
Along with antiviral drugs, ganglion blockers, such as Gangleron, are used to reduce pain. Gangleron is used intramuscularly in the form of a 1.5% solution, 1 ml once a day for 10–12 days or 0.04 g in capsules 2 times a day for 10–15 days, depending on the severity of the pain syndrome. In addition, the use of carbamazepine gives good results, especially in cases of damage to the Gasserian node; the drug is prescribed with 0.1 g 2 times a day, increasing the dose by 0.1 g per day, if necessary, up to 0.6 g daily dose (in 3– 4 doses). After the pain decreases or disappears, the dose is gradually reduced. Usually the effect occurs 3-5 days after the start of treatment.
In cases of severe pain, analgesics and, in the form of injections, reflexology are prescribed. In reflexology, both points of general action and points corresponding to the affected ganglion are usually used. The course consists of 10–12 sessions. It is also recommended to prescribe multivitamins, in particular B vitamins. Local irrigation with interferon or ointments with interferon, aniline dyes, Eridin aerosol, Florenal, Helepin, Alpizarin ointments can be used. For gangrenous forms of herpes zoster, pastes and ointments containing an antibiotic, as well as Solcoseryl, are used.
Good results are obtained by irrigation with Epigen spray 4–5 times a day for 7–10 days from the first days of the disease. When combined with oral acyclovir therapy, a decrease in pain is noted.
After the skin rash resolves, treatment is carried out by neurologists until the neurological symptoms disappear.
Thus, treatment of herpes zoster should be comprehensive and include both etiological and pathogenetic agents.
Literature
- Batkaev E. A., Kitsak V. Ya., Korsunskaya I. M., Lipova E. V. Viral diseases of the skin and mucous membranes. Textbook manual, RMAPO. M.: Pulse, 2001.
- Butov Yu. S. Skin diseases and sexually transmitted infections.
- Kartamyshev A.I. Skin and venereal diseases. Medgiz, 1954.
- Skin and venereal diseases: Directory. Ed. O. L. Ivanova. M.: Medicine, 1997.
- Paltsev M. A., Potekaev N. N., Kazantseva I. A. et al. Clinical and morphological diagnosis of skin diseases (atlas). M.: Med., 2004.
- Pospelov A.I. A short textbook of skin diseases. M., 1907.
- Skripkin Yu. K., Kubanova A. A., Prokhorenkov V. I. et al. Dermatological syndromology. M. - Krasnoyarsk, 1998.
- Sukolin G.I. Clinical dermatology. St. Petersburg, 1997.
- Lezvinskaya E. M., Piven A. L. Laboratory diagnostics: skin diseases and sexually transmitted infections. M.: Practical Medicine, 2005
- Yushchuk N. D., Stepanchenko A. V., Dekonenko E. P. 2005.
- Kalamkaryan A. A., Kochetkov V. D. 1973.
- Zucker M. B. 1976.
I. M. Shakov, Candidate of Medical Sciences
GOU DPO RMAPO, Moscow
Contact information about the author for correspondence
Fungal infections
Ringworm is contagious. In case of a fungal infection, it is important to know how to understand that a person’s lichen is going away in order to exclude the transmission of infection. New lichen is characterized by an increase in the size of the spots, the presence of a bright pink ridge of skin along the contour, in the center the skin is covered with small blisters that burst and become flaky scales. Ringworm affects the hair, causing it to break off at 2-4 mm near the root. As a result, bald spots appear.
The first signs of healing lichen are changes associated with a decrease in foci of inflammation:
- The spots stop growing in diameter.
- The skin gradually dries out.
- Light new skin appears under the falling scales.
- The ridge surrounding the lesion becomes less bright and also peels off.
It is important to understand that the lichen has passed and is no longer contagious to people. Therefore, the dermatologist performs three repeat tests. Even if the skin structure is restored, taking drugs against fungal infection continues for another 2-3 weeks to prevent relapse, after which the examination is repeated again. Scrapings are taken from the affected areas three times - every 2-3 weeks - to exclude the appearance of live fungi. The effectiveness of therapy is indicated by a triple negative test result. Even if one microorganism is detected, it is necessary to continue the course of drugs again.
Self-examination of the affected areas also helps. The skin should be smooth to the touch, indistinguishable from healthy tissue, and not have roughness or bumps.
Other diagnostic methods
Pityriasis versicolor is caused by fungi, but differs from other types of disease visually. The skin in the affected areas has an uneven and loose texture. The shape of the lesions is varied. These may be round spots or irregularly shaped areas that merge into one large lesion.
Diagnosis at an early stage is carried out with the help of iodine, using the Balzer test - it consists in the fact that when an iodine solution is applied, the spots become darker and more visible.
The stratum corneum of the skin loosens due to the activity of the fungus, and more of the coloring solution is absorbed. Places where lichen is present become brown, but untouched areas remain light.
The iodine test makes it easy to track the progress of treatment. If there are fewer dark spots after applying the solution, then recovery is recorded. In fact, the disease persists while the affected areas grow.
Dermatologists use scraping cultures. Under a microscope, threads of fungus and living cells are detected in the collected sample, which indicates the need for treatment.
Another diagnostic method is examination under the rays of a Wood's lamp or a UV quartz lamp. Foci affected by the fungus are distinguished by brown, green or yellow-red shades.
Healing of viral lesions
The Herpes virus, responsible for shingles, becomes active in the form of cold symptoms. First, the patient experiences chills, malaise due to increased temperature, burning and tingling in the intercostal spaces, where the rash is usually localized. After three days, red, inflamed spots turn into vesicles, which open as they mature and dry out. In place of the peeled crust, spots with altered pigmentation remain, this is how healing of herpes zoster is noted. However, time must pass for complete relief from pain.
Skin diseases often cause a person to feel discomfort, itching, burning, which needs to be gotten rid of, so you should know what pityriasis rosea is in humans - symptoms and treatment methods. Diseases of this type are very similar to each other, so to determine the type you need to contact a dermatologist. Such diseases are not life-threatening, but they cannot be left untreated. They use medications and traditional medicine.
Pityriasis rosea in children
Children suffer from this pathology much less often than adults; the disease most often affects people aged 4-12 years. Zhiber's pityriasis rosea in most cases occurs in girls; before the appearance of the rash, signs of a cold are observed. With further development, the symptoms do not differ from adults. Pityriasis rosea in children develops when the body's defenses are reduced, but recovery occurs without specific treatment. For treatment of lichen, a dermatologist may advise:
- the use of antihistamines (Loratadine, Suprastin, Fenistil) if severe itching is present;
- restriction on the period of treatment of water procedures to prevent the spread of stains;
- taking vitamin complexes;
- limiting sun exposure;
- wearing clothes and underwear only made from natural fabrics;
- exclusion of citrus fruits, chocolate, honey, nuts, eggs from the diet.
Why does pityriasis rosea appear in humans?
The main causes of the disease are not fully understood. It is believed that a viral infection becomes the main causative agent, similar to herpes type 6, 7. This explains why the disease manifests itself in autumn and spring (immune defense sharply decreases). This theory is also supported by the fact that flu symptoms appear along with the rash. Another option for why pityriasis rosea appears in humans is an allergic reaction, often while taking medications. Doctors admit the following possibilities of infection:
- contact – through things in common use;
- airborne;
- with an insect bite.
The likelihood of developing pathology is also influenced by the following factors:
- intestinal diseases;
- vaccination;
- metabolic disorders.
If a person strengthens his immune system, then the likelihood of developing a rash is extremely low. According to other studies, the causes of pityriasis rosea can be:
- skin reaction to low temperature due to weak immune defense;
- fungi;
- infectious-allergic reaction to an irritant;
There are also external factors that can trigger the appearance and spread of pityriasis rosea:
- overheat;
- prolonged nervous tension, severe stress;
- bathing in hot water.
Diagnosis of pityriasis rosea in humans
If itchy spots and similar symptoms are detected, a person tries to self-medicate, relying on photographs. Only an experienced doctor knows what pityriasis rosea looks like and can distinguish it from other skin diseases. If you use the wrong tinctures, oils or ointments, you can aggravate the pathology and make it worse. Diagnosis of pityriasis rosea in a person is the first step towards recovery. Differentiation of symptoms of the disease simplifies the treatment process. To clarify the pathology, the following diseases are excluded or confirmed using scraping microscopy:
- ringworm;
- dermatomycosis (fungus);
- microsporia;
- pityriasis versicolor.
All these diseases have similar external manifestations to pityriasis rosea. In addition to the above, you can confuse Gibert's pityriasis with:
- secondary form of syphilis;
- eczema;
- HIV infection;
- psoriasis;
- allergic reaction of the skin to an irritant.
Often, based on external symptoms, people confuse pityriasis rosea with pityriasis versicolor, which is also common. The main difference between them is that after Zhiber’s disease an even tan remains at the sites of the rash, while after pityriasis there are white spots. Antifungal agents are effective in treating the multicolored form of the disease. Another distinctive symptom of Zhiber’s disease is that a rash appears in the natural folds of the body.
Prognosis and prevention
Since it has not yet been possible to identify the causative agent of Zhiber's disease, prevention is of a general nature. Doctors recommend:
- Dress appropriately for the weather and avoid hypothermia.
- Treat viral infections promptly and completely. After recovery, take a course of vitamin therapy.
- If you cannot avoid stressful situations, take sedatives to prevent possible complications.
- Constantly support your immune system: eat protein foods, walk in the fresh air, play sports, and exercise.
- Observe personal hygiene rules.
- Eat right and minimize the consumption of foods with preservatives.
Pityriasis rosea does not cause dangerous complications and does not have a negative effect on the body as a whole, so treatment prognosis is always favorable. Even if you do not use drug therapy, Zhiber's disease will go away on its own over time, and the patient will acquire stable immunity and will never suffer from characteristic skin reactions.
Eczema
Eczema is another unpleasant skin disease characterized by inflammatory processes on the human skin. In most cases, it begins in childhood, and adults usually get it only if it was treated incorrectly in childhood, and by its nature it has developed into a chronic illness.
Eczema has the following symptoms:
- at the site of inflammation, the skin becomes reddened (occasionally blue), slightly thickened;
- gradually a rash forms at the site of inflammation, often with blisters of liquid;
- the skin itches unpleasantly, up to a constant, incessant effect;
- when the blisters are damaged, the skin in their place becomes covered with wounds and cracks;
- possible increase in body temperature;
- after the inflammation has passed, the skin remains dry and very susceptible to cracks.
The disease can appear on any part of the body, but according to statistics, the arms (in particular, the palms) and legs are most often affected.
Photo showing the manifestation of eczema
We present a photo of eczema to distinguish it from other diseases.
How to quickly cure pityriasis rosea
There are several methods for treating Gibert's disease. All of them are aimed at eliminating symptoms and preventing possible complications (addition of secondary infectious and inflammatory diseases of the skin).
Whatever therapeutic direction is chosen, the patient must adhere to the following recommendations:
- Do not wet or rub stains with washcloths or take hot baths. Any heating contributes to the further spread of the rash. Patients are allowed to shower and use cleansers that do not dry out the skin.
- It is worth limiting your exposure to the sun.
- It is important to temporarily stop wearing synthetic clothing and items made from fabrics with added wool.
- You should not walk around sweating for a long time: salt increases skin irritation.
- It is advisable to adhere to the rules of restrictive nutrition. Products that can cause allergies (honey, eggs, chocolate, nuts, citrus fruits) should be prohibited. It is important to avoid dishes that contain preservatives, flavor enhancers, and chemical dyes.
Dermatitis
Dermatitis is also an inflammatory skin disease. Skin damage by dermatitis occurs due to exposure to irritating substances, depending on which one or another form of the disease manifests itself.
Dermatitis can be of the following types:
- Seborrheic dermatitis. It is caused by a fungus, but is not contagious to others. It is chronic and appears on the skin of the face and scalp. Main symptoms: the appearance of greasy yellow scales and crusts.
- Contact dermatitis. Appears after exposure to external irritants of various types on the skin. Red spots and a rash appear, accompanied by itching and burning, and sometimes pain.
- Allergic dermatitis. Occurs chronically. Swelling, rashes, and erythema appear.
- Atopic. It is also chronic, more severe than others, and occurs in people who are predisposed to atopy. Manifests itself in the form of inflammation, red swelling, and blisters with liquid.
Photo of dermatitis
To understand what red spots look like with this skin disease, we suggest looking at a photo of dermatitis.
Infections
Sometimes red spots on the skin indicate the presence of a certain infectious disease.
Such diseases include:
- chickenpox;
- scarlet fever;
- rubella;
- measles;
- venereal diseases (syphilis).
In any case, to find the right treatment, you need to see a doctor.
Photos of manifestations of infectious diseases
Traditional methods of getting rid of skin spots
There are, of course, traditional methods for treating certain skin diseases:
- Dermatitis is treated by using an infusion of burdock and dandelion. A tablespoon of plant roots is infused overnight in three glasses of water, and boiled in the morning. Drink half a glass, 5 times a day, for 3 weeks.
- Eczema is treated by drinking concentrated lemon juice or infusion of gentian and yarrow.
- Allergies are treated simply by removing the allergen from a person’s environment.
- Ringworm can be treated with chamomile - consumed as tea, or made into compresses. Baths with oatmeal, as well as applying kefir or sour cream to the stains, also help.
- Pigment spots are treated with a mask of green parsley.