Erysipelas, or simply erysipelas, is an infectious-allergic disease that affects the skin and subcutaneous tissue. The disease is quite common and prone to relapse. It ranks fourth among all infectious diseases and is also becoming more common over time. Thus, over the past twenty years, the number of relapses of this disease has increased by 25%. Moreover, a severe form of the disease is becoming more common - now it is about 80% of cases, although 50-60 years ago only 30 percent of patients were diagnosed with a severe form.
At-risk groups
Most often, women over 50 years of age are affected by this disease, but it can also occur in infants. In their case, infection occurs after streptococcus enters the wound of the umbilical region. There is no explanation for this fact, but people with blood group III suffer from erysipelas more often. There is also a connection with the place of residence. In South Asia, as well as in Africa, this disease is very rare.
People with a low level of immunity, weakened by illness, stress, treatment and other factors are at risk.
Symptoms
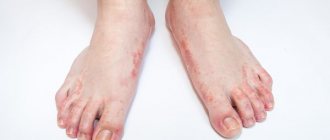
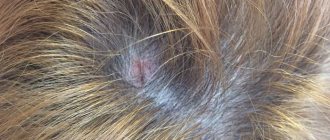
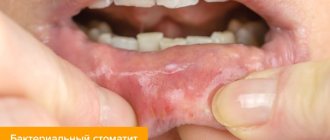
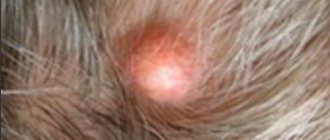
You can notice the first symptoms of erysipelas on different parts of the body: legs, arms, face, torso, perineum. Moreover, much will depend on how exactly the disease develops. For example, inflammation on the face can be localized around the eye socket, near the ear, on the scalp and neck. If the disease starts from the nose, a butterfly-type lesion may develop - extending to the cheeks. At the same time, swelling occurs, which distorts the size of the tissue. The same applies to all other organs - the localization of the disease is different and depends on the situation.
Symptoms of erysipelas are divided into general and local. General points include:
- Chills, fever. Patients often shake violently.
- High temperature, up to 40 degrees. It can last up to ten days.
- Convulsions, clouding of consciousness, delirium.
- Very strong weakness, dizziness.
- Nausea, often vomiting.
- Pain in muscles and joints.
In other words, symptoms of general poisoning of the body are observed.
Local symptoms of erysipelas look like this:
- Redness of the skin at the site of the lesion. Usually changes are noticeable ten to twenty hours after the pathological processes begin.
- Puffiness, swelling, pain in the place where the skin rises. Also, the area of skin becomes warmer to the touch, even hot. The patient may feel a burning sensation and a sensation as if something is bursting the skin from the inside.
- Rapid growth of inflammation, since streptococci multiply quite actively. The edges of the lesions are uneven, they constantly change as they grow.
- Enlargement of nearby lymph nodes as the pathogen spreads through the lymphatic system.
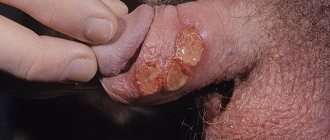
- Bubbles with clear liquid. They are small at first, but then they grow and unite with each other. This sign is not always present.
- Hemorrhages. If you do not help the patient at first, complications will occur, including damage to the blood vessels, the blood of which enters the intercellular space.
- Bubbles with blood and pus surrounded by areas of hemorrhage. The classification of erysipelas suggests different degrees of development of the disease - and these manifestations are already characteristic of complicated forms.
The more advanced the situation, the higher the risks that even after successful treatment a relapse will occur. Often the disease occurs in the same place as the first time.
Preventive measures for erysipelas
Prevention of injuries and abrasions of the legs, treatment of diseases caused by streptococcus.
Frequent relapses (more than 3 times a year) in 90% of cases are the result of a concomitant disease. Therefore, the best prevention of the second and subsequent occurrences of erysipelas is treatment of the underlying disease.
But there is also drug prevention. For patients who regularly suffer from erysipelas, there are special long-acting (slow) antibiotics that prevent streptococcus from multiplying in the body. These medications must be taken for a long time, from 1 month to a year. But only a doctor can decide whether such treatment is necessary.
Causes
Erysipelas is caused by streptococci - or rather, one of the varieties of bacteria of this group. In an organism with a weakened immune system, streptococcus can cause other diseases - for example, scarlet fever, myocarditis, and sore throat.
About 15% of the world's people are carriers of streptococcus. That is, their immunity is quite strong so as not to get sick, but at the same time they spread the infection. It is transmitted through personal contacts, household objects, airborne droplets, etc.
Predisposing factors for infection:
- Various skin injuries, including insect bites, animal bites, bedsores and ulcers. Even venous catheters can be dangerous in this sense.
- Harmful working conditions - when the skin is constantly exposed to chemicals, it often becomes dirty. People who constantly wear rubber clothing and shoes are also at risk.
- Viral skin lesions - chickenpox, shingles, herpes. They not only violate the integrity of the integument, but also greatly reduce immunity.
- Chronic skin lesions such as eczema, atopic dermatitis, psoriasis, etc.
- Purulent lesions of the skin: boil, carbuncle and similar formations.
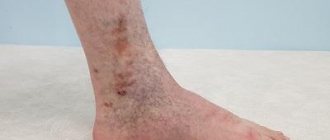
- Disturbances in the circulatory system - varicose veins, thrombophlebitis. If the skin is deprived of oxygen, it becomes damaged and becomes more susceptible to infection.
- Various scars, the cells of which the body itself can attack, which is why erysipelas develops.
- Fungal diseases of the scalp and feet.
- Serious complications with rhinitis, otitis media, conjunctivitis.
- Injuries to the skin caused by wearing tight clothing that rubs and disrupts blood circulation in the tissues.
- Any reasons that suppress the immune system: taking certain medications, serious illnesses, exhaustion as a result of malnutrition, hypothermia, bad habits, chronic or severe stress and much more.
To summarize, the disease develops against a background of weakened immunity and streptococcal infection, which can occur in different ways.
What is erysipelas
This is a common bacterial infection of the mucous membranes or skin with the development of limited serous foci of inflammation. The disease is often accompanied by fever and symptoms of general intoxication. Occurs at any age. The causative agent of the process is streptococcal infection. This can be its own conditionally pathogenic microflora or microbes obtained from outside. The risk of erysipelas increases:
- for mechanical injuries to the skin: scratches, scratches, scars, cicatrices;
- for acute or chronic tonsillitis;
- in the presence of carious teeth;
- for runny nose and sinusitis;
- with hypovitaminosis.
Damage to the skin and mucous membranes by streptococci is favored by unsanitary conditions: infrequent hand washing, neglect of personal hygiene rules. It has been established that in the warm season, erysipelas occurs more often. Infection is also facilitated by surges in immunity and the use of certain medications, for example, immunosuppressive or steroid hormones.
Diagnostics
If the first signs of erysipelas occur, you should consult a dermatologist or therapist. Depending on the extent of the problem, assistance from specialists such as an immunologist, surgeon, or infectious disease specialist may be required.
Diagnosis of the disease includes interviewing the patient, as well as a thorough examination. Then tests are prescribed for the level of T-lymphocytes, ESR, and the number of neutrophils (all this is determined through a blood test).
An optional bacteriological examination is prescribed to determine the causative agent - doctors do not agree on the advisability of such an examination.
Treatment
If erysipelas develops on a leg, arm or other part of the body, the approach will always be comprehensive - local treatment alone is simply not enough. Moreover, the emphasis is largely on increasing immunity, otherwise the risks that the disease will recur are very high. Special medications are used to work with the immune system, but it is important for the patient to change their lifestyle: rest well, carefully monitor their health, eat right, and eliminate negative factors.
In the treatment of erysipelas, antibiotics are used, as well as antibacterial drugs from other groups. Drug therapy is selected individually - you should not prescribe medications yourself under any circumstances.
Along with taking medications, it is necessary to treat the affected skin: with special solutions, powders, aerosols. And the ointments that people love to prescribe for themselves - synthomycin, ichthyol, Vishnevsky - are strictly prohibited in this case, since they can provoke complications and cause the development of an abscess. The use of traditional medicine in any form is not allowed - in the treatment of erysipelas it is extremely dangerous!
Patients must have a preventive conversation regarding the nuances of hygiene during treatment. So, you need to change bed linen every day, take care of air access to the affected area, and regularly take a shower in warm, very comfortable water. Do not wipe the skin - only soak it with paper towels.
Physiotherapeutic methods are also used for erysipelas: ultraviolet irradiation, magnetic therapy, UHF, electrophoresis, certain types of laser therapy, applications with warm paraffin. At each stage of treatment, specific procedures are prescribed, and they are selected individually - for each patient and his condition. Any amateur activity is also inappropriate here, otherwise you can harm your health.
Very serious complications require surgical treatment.
If you encounter such a problem, we recommend immediately contacting the JSC Medicine clinic. We are located in Moscow and have a large staff of professional dermatologists, therapists and other specialists who can help you. And modern conditions for diagnosis and treatment will help achieve results much faster.
If doctors begin treatment in a timely manner and the patient follows all recommendations, the disease can be cured within 10-14 days.
Complications and consequences of the disease
In children, the elderly, and people with venous insufficiency, erysipelas is more severe, often lasts up to 1 month or more, and is prone to relapse and become chronic. In acute periods, the disease threatens loss of consciousness and coma. Common complications of erysipelas include:
- inflammation of the veins - phlebitis;
- formation of trophic ulcers, abscesses, phlegmons;
- development of sepsis;
- the consequences of hemorrhagic and bullous forms are scars.
Sometimes erysipelas provokes subsequent hyperkeratosis, eczema, elephantiasis - chronic swelling of the lower extremities.
Prevention
Since the disease can affect anyone, prevention of erysipelas is important both for those who have already had the disease once, and for those who have only heard about such a disease.
Prevention consists of following the following tips:
- Treat any inflammation on the skin or mucous membranes in a timely manner.
- Maintain personal hygiene. In the event that work or lifestyle is associated with additional pollution, hygiene should be even more thorough, but not excessive, so that the skin does not suffer - otherwise the effect will be the opposite.
- Use special products (gels and oils) for washing that do not dry out the skin. Regular soap is not suitable for regular use.
- Carefully monitor the condition of your skin in hot weather or if you have folds that constantly sweat. In this case, it is necessary to use special powders.
- Pay close attention to your health if you have problems with blood vessels or lymph stagnation. Such people are recommended for massages and various procedures that disperse fluids in the body.
- Treat your skin immediately if you have frostbite, chapping, or sunburn.
- Wear comfortable, breathable, natural clothing if possible that fits loosely on the body.
- Carefully monitor your immunity and eliminate all factors that can weaken it.
Remember that you cannot insure against this disease, but you can do everything to reduce the risks of its occurrence.
Erysipelas due to lymphedema
Erysipelas is a bacterial hypodermal cellulitis that is usually associated with streptococcal infection. Most often it is a complication of chronic lymphedema. The first signs are a sudden rise in temperature and chills. The clinical feature is an inflammatory dermatitis with clearly defined boundaries, which is often accompanied by fever. Inflammatory skin thickening contributes to lymph stagnation and the progression of lymphedema.
Erysipelas, as such, is mainly treated with antibiotics. Relapse prevention is an important goal. Because lymphedema is a major risk factor for recurrence, aggressive treatment is necessary.
Risk factors for erysipelas
The lymphatic system plays an important role in protecting the body from infection. Stagnation of lymph during lymphedema contributes to the penetration of infection into dilated lymphatic capillaries. Infectious complications are mainly bacterial, most often erysipelas (cellulitis), and sometimes lymphangitis (inflammation of the lymphatic vessels). The most common causative agent of erysipelas is β-hemolytic streptococcus (groups A, C, G). Bacterial complications are facilitated by the abundance of proteins characteristic of edema in lymphatic insufficiency associated with obstructed lymphatic drainage. This high protein content in the interstitial fluid provides an ideal breeding ground for bacterial growth.
Erysipelas is a dermo-hypodermal bacterial infection without involvement of the superficial aponeurosis. Erysipelas complicates lymphedema in 30% of cases and aggravates its course.
With lymphedema, chronic inflammation of the skin is very common; it may not be associated with infection, but only with stagnation of lymph. However, the presence of streptococcus in changed skin is always a risk factor for erysipelas. And the use of hormonal ointments on the skin of patients with lymphedema can provoke deep purulent-necrotic damage to the subcutaneous tissue and fascia.
Symptoms
Erysipelas often occurs suddenly, with pronounced systemic signs - fever >38 ° 5, chills and general malaise. Local signs develop within a few hours: redness, local fever, pain and rapid spread of the lesion, with centrifugal expansion over several days. Erysipelas can begin at any stage of lymphedema and can spread to all or part of the changed skin tissue.
Diagnosis
The diagnosis of erysipelas is established clinically:
The sudden onset of an inflammatory lesion that spreads over several days, preceded or accompanied by fever and chills, as well as general malaise.
Streptococcus is isolated only from 4% to 35% of cases in patients with erysipelas. If the most sophisticated methods are used (immunofluorescence, polymerase chain reaction), then streptococcus is isolated with a frequency of 70% to 80%.
Differential diagnosis
Erysipelas must be differentiated from other infections sometimes seen with lymphedema, such as lymphangitis, most often streptococcal (less commonly staphylococcal) or necrotizing fasciitis (most often streptococcal).
Lymphangitis is characterized by the appearance of an inflammatory streak (red, hot and painful) along the superficial lymphatic vessels (which themselves are satellites of the superficial venous system). Accompanied by fever. There is no spread of the lesion into deep tissues.
Other acute forms of dermo-hypodermal bacterial infections are caused by Erysipelotrix rhusiopathiae (swine erysipelas), the bacterium pasteurella multocida, and borrelia borgdorferi. They have a less inflammatory and febrile clinical presentation without the typical chronology of erysipelas.
Thus, the diagnosis of erysipelas is purely clinical in nature and does not require any laboratory tests, in particular bacteriological ones.
Treatment
Antibacterial treatment is carried out with amoxicillin tablets (3-4.5 g/day, in 3 doses) for two weeks.
Hospitalization is necessary if:
- There is doubt about the diagnosis, or there are serious systemic features, comorbidities, or a social context that makes home treatment impossible for the patient.
- Fever persists for more than 72 hours. In such cases, treatment is carried out with intravenous penicillin g (10-20 million units in 4-6 infusions per day).
Relapse Prevention
Erysipelas with lymphedema often recurs and aggravates its course. To avoid recurrence of erysipelas, treatment is carried out with long-acting penicillins. (Extencillin or Retarpen 1 gram per week for 4 weeks during a possible exacerbation).
Treatment of lymphedema using conservative and surgical methods, maintaining the disease without progression helps reduce the likelihood of relapses of erysipelas.